Laparoscopic Anti-Reflux Surgery
Laparoscopic anti-reflux surgery - sometimes referred to as fundoplication - is one of the most common surgical treatments for gastro-oesophageal reflux disease (GORD).
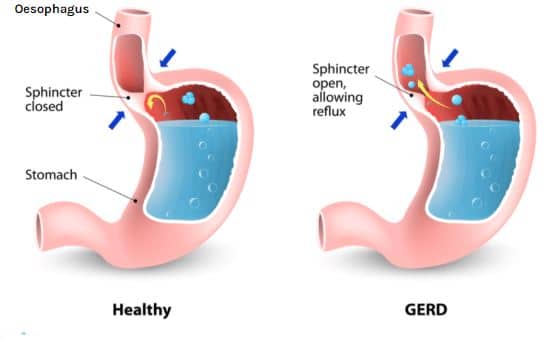
GORD is a disease which involves inflammation and pain that is the result of acid (and sometimes bile) refluxing into the oesophagus from the stomach. One of the main causes can be the malfunctioning of the 'barrier' which prevents acid reflux - that is, the lower oesophageal sphincter which is made of a number of anatomical structures (muscles and ligaments) that can fail.
The most common anatomical failure causing acid reflux is the presence of a hiatus hernia - caused by a widening of the diaphragm. Acid reflux is a complex condition sometimes caused by poor function of the oesophagus (AKA as food pipe or gullet); when the oesophagus doesn’t contract effectively the gastric acid spends too much time in contact with the oesophagus causing oesophagitis (inflammation of the oesophagus) and with time Barrett’s oesophagus (pre-cancerous condition).
Because laparoscopic anti-reflux surgery can achieve the strengthening of the lower oesophageal sphincter which provides this barrier, it can help to combat the problem of GORD and acid reflux.
Laparoscopic anti-reflux surgery is typically considered a viable treatment path for GORD patients who have not responded satisfactorily to drugs intended to suppress stomach acid. This is usually a minority of those who suffer from acid reflux. Other candidates for laparoscopic anti-reflux surgery might have experienced intense side effects from medication, or have opted for surgery in order to eliminate the need for medication.
The laparoscopic anti-reflux surgery procedure itself - which typically takes between one hour and 90 minutes - is conducted using keyhole techniques (5 small cuts in your abdominal wall) which are minimally invasive compared to forms of open surgery.
The fundus of the stomach - which is the part of the stomach closest to the oesophagus entry - is gathered and wrapped, before being stitched around the oesophagus' lower end. Because this serves to increase the pressure level at the lower part of the oesophagus, acid reflux can be reduced. The wrapping of the fundus recreates a high-pressure zone‘, which prevents stomach acid from refluxing up to the oesophagus.
It is common for GORD patients to have suffered a hiatus hernia which is associated with the condition, and a hernia repair can be undergone at the same time as laparoscopic anti-reflux surgery.
A Fundoplication is not free of side effects and complications. The most common side effect is called gas bloat syndrome and is caused by the change in shape of the stomach. This will be reduced in side (despite nothing is removed during a fundoplication) and food will pass into the small bowel much earlier. The food bolus once in the small bowel will trigger strong contractions of the bowels resulting in cramps, flatulence and loose stools.
These symptoms can be as common as in 30% of the patients and can be improved with changes in the diet and medications.
The second most common side effect/complication is dysphagia (difficulty swallowing). Most of the time it is a self-resolving problem caused but the inflammation caused by the operation and lasts 4-6 weeks. In approximately 10% of the patients an endoscopy is required to widen the fundoplication and in 1% a re-operation may be needed.
What are the advantages of having laparoscopic anti-reflux surgery?
- Laparoscopic surgery is minimally invasive.
- There is a better cosmetic result compared to open forms of surgery.
- Recovery is faster and there is less post-op pain compared to open forms of surgery.
- There is a low risk of complications from laparoscopic anti-reflux surgery.
- According to figures published by the NHS, laparoscopic anti-reflux surgery "improved or eliminated heartburn and regurgitation in more than 90% of patients".
- Laparoscopic anti-reflux surgery is also capable of curing GORD-induced respiratory or asthmatic symptoms in a high proportion of patients.
Positive lifestyle steps which can help you prepare for surgery include:
- Taking regular exercise (aim for 30 minutes a day). This could be a simple walk, a more rigorous workout, or playing sports.
- Improving your diet, reducing your calorie intake, and make sure you are drinking lots of water.
- If you are a smoker, try to quit for at least two weeks prior to the operation.
- Try to refrain from drinking alcohol for at least two weeks prior to the operation.
Contact Us
